an HIV TELEHEALTH TRAINING PROGRAM supplemental session
In March 2020, we were one of the first organizations in the Philippines to conduct a series of webinars on HIV and COVID related topics, as a supplemental learning for the HTTP graduates. The webinars were developed as a way to ensure the continuity of care for People Living With HIV (PLHIVs) and at-risk groups during the COVID-19 pandemic & ensuing lockdowns.
This webinar series greatly benefitted our HTTP graduates, as well as other primary care workers, by providing timely knowledge and awareness in order to adapt and respond to the challenges brought upon by the pandemic.
This year, as the Philippine government is about to roll out a national vaccination program against COVID-19, we are at a critical point where knowledge must be shared to HIV healthcare providers, and vaccine confidence boosted among PLHIVs, while focusing on the latest science and updates on HIV and COVID-19 vaccines.
Here are the Q&A topics that followed:






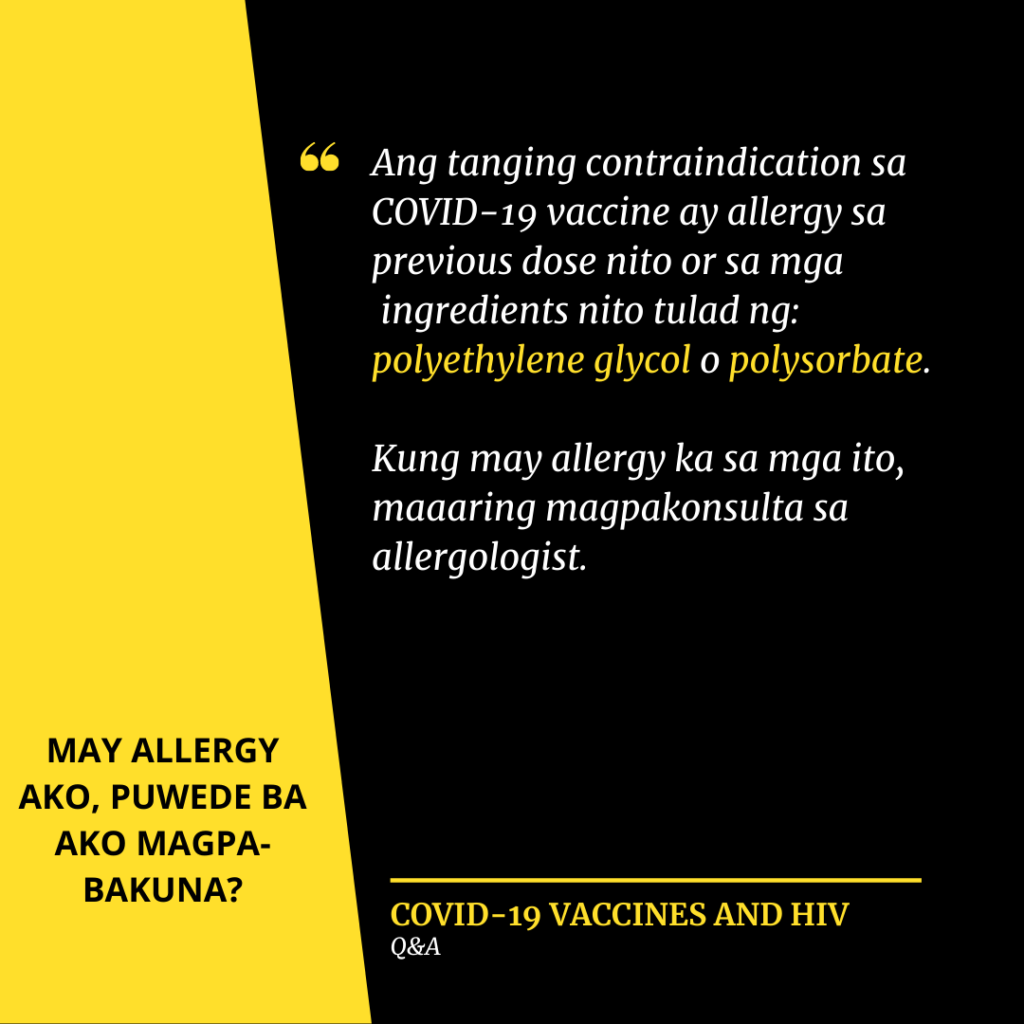




The most common question sent in by attendees was whether special provisions were to be made for PLHIV for easier access to the vaccine. Worries about confidentiality, disclosure, and unnecessary exposure to the public of immunocompromised individuals were the reasons given for desire for a more localized area of distribution.
We will follow up with the Department of Health for a statement regarding this concern.